Scan Planes: - Upper abdominal transverse scan (to demonstrate the left lobe)
- Right subcostal oblique
- high and extended right intercostal scans.
- paramedian upper abdominal longitudinal scans.
Sonographic Anatomy and Normal Findings:
- The liver exhibits a diaphragmatic surface and a visceral surface.
- Both surfaces meet anteroinferiorly at the sharp inferior hepatic border and posterosuperiorly at the fixed part of the diaphragm.
- The liver is divided anatomically into the right and left lobes, the falciform ligament separating the larger right lobe from the smaller left lobe. The quadrate lobe (segment IV) and the caudate lobe (segment I) belong physiologically to the left lobe.

Segmental anatomy of the liver, diaphragmatic surface. A line between the gallbladder and inferior vena cava divides the liver into right (Segment V–VIII) and left physiologic lobes (Segment I–IV)

Segmental anatomy of the liver, visceral surface. Boundaries of the caudate lobe: upper hepatic border, falciform ligament, portal vein, and vena cava. Boundaries of the
quadrate lobe: lower hepatic border,
falciform ligament, gallbladder,
and portal vein
Scanning Protocol
- Transducer: 2.5–5.0 MHz (depending on the abdominal circumference)
- Right subcostal oblique scan: Ask the patient to take a deep breath and hold it.
- Define the dome of the liver with the diaphragm, hepatic veins, portal venous branches (common hepatic duct), the intrahepatic bile ducts, the gallbladder, and the hepatic parenchyma.


Subcostal oblique scans. Scan through the porta hepatis into the upper part of the liver. PV = right and left branch of the portal vein. V = inferior vena cava, arrow = ligamentum venosum.


Scan directed from the inferior hepatic border (at top of image) to the fixed part (at bottom of image) demonstrates
the quadrate lobe (QL) and caudate lobe (CL) anterior to the vena cava (VC). L = right lobe of liver, PV = portal vein
Schmidt, Ultrasound


Upper abdominal longitudinal scan of the subdiaphragmatic vena cava and the termination of the hepatic veins (arrow). QL = quadrate lobe, PV = portal vein, CL = caudate lobe, VC = inferior vena cava, L = liver


High intercostal scan on the right side demonstrates the costophrenic angle (CA), posterior portions of the diaphragm (DIA) and the entry echo of the lung (L)
Overview of Findings, Classification:
Changes in the liver: Sonographic abnormalities of the liver may consist of diffuse or circumscribed changes in the normal hepatic architecture:
Diffuse changes: These refer to a general alteration of normal liver architecture with regard to size, echogenicity, contours, vasculature, and tubular tracts. Changes in echo texture and contours are particularly significant.
Circumscribed changes: focal alterations in the normal echo texture of the liver. Their detectability depends on the difference in acoustic impedance between the change and normal surrounding liver (anechoic lesions such as cysts are easily recognized). A lesion that is isoechoic to surrounding liver can be distinguished only by the presence of a hypoechoic rim or vascular displacement
Changes in the portal veins: Abnormalities of the portal vein and its tributaries may produce changes identical to those found in the systemic veins.
Diffuse changes in hepatic echogenicity or contours

Circumscribed hepatic changes

1) Fatty Liver


Slight coarsening of the parenchymal echo pattern, increased echogenicity, distal acoustic shadowing, and organ enlargement
2) Chronic Hepatitis


Very slight coarsening of the parenchymal echo pattern and
increased sonodensity with faint acoustic shadowing.
Right subcostal scan
Congestive cirrhosis


Congestive cirrhosis. The liver still has a near normal parenchymal
Echo pattern, but note the curved, bulging inferior border and the tiny
breaks in the capsule (arrows). A = ascites
Very Pronounced changes in echogenicity and contour
1) Sarcoidosis


Sarcoidosis of the liver: coarse parenchymal echo pattern, nonvisualization of
the vessels, and multiple small hypoechoic foci (arrows)
2) Micronodular abscesses or metastases

Micronodular infiltrates in the liver
Anechoic Changes
1) Liver cysts
Solitary Cyst in Liver
 Septated Cysts in Liver
Septated Cysts in Liver

Cystic Echinococcosis

Hypoechoic Changes on Liver Ultrasound
1) Focal Sparing in Fatty Infiltration of Liver

Hypoechoic quadrate lobe (segment IV, arrows) adjacent to the gallbladder (GB) in an otherwise fatty liver
Regenerative nodule in severe alcoholic toxic cirrhosis (arrow), confirmed cytologically
3) Hemorrhagic Liver Cyst

4) Liver abscess
Hypoechoic, sharply circumscribed mass with a faintly Echogenic wall

Hyperechoic pyogenic membrane is often present
5) Adenoma

Isoechoic tumor with focal anechoic necrosis / hemorrhage.
Isoechoic Changes in Liver
1) Liver Metastases

The lesions are demarcated from normal liver tissue only by a hypoechoic rim (this accounts for a certain percentage of sonographically occult metastases that are detectable by other modalities).
Echogenic and Hyperechoic Changes

Hemangioma (H) of the liver (L): typical Echogenic, round to oval mass with smooth margins.

Metastasis from colon carcinoma: echogenic round mass with a less echogenic center.

Calcifying metastasis from colorectal carcinoma
Changes in the Portal Venous System
1)Changes in Portal Vein Lumen – Dilatation.
Commonest finding of Portal Hypertension.
But the diagnosis also relies on CDS(colour doppler) and flow patterns across the portal vein lumen
Common causes of Portal Hypertension are: Pre Hepatic – Portal Vein Thrombosis
Intra Hepatic – Cirrhosis
Post Hepatic – Budd Chiari Syndrome
Increased portal vein diameter, indirect signs: - > 11mm intrahepatic, > 13–15mm in the hepatoduodenal ligament
- Caliber variations I 2mm or 50–100 % with respirations
- Detection of hepatic cirrhosis
- Splenomegaly
- Possible ascites
- Wall thickening of the gallbladder and stomach
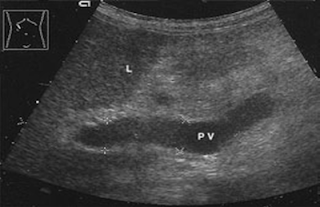
Incipient portal hypertension. The portal vein (PV) is marginally dilated: 12.9mm intrahepatic
2) Flow Changes and Collaterals:
- Associated with increased portal hypertension.
- Detected on CDS of portal vessels.
Flow velocity is slowed to < 10 cm/s (normal = 15–20 cm/s)
Luminal diameter > 15 mm, does not vary with respirations
Bidirectional, absent or reverse flow in the portal vein or its tributaries


Portal hypertension in liver cirrhosis. CDS: decreased flow velocity
with absence of flow in the portal vein. Flow is in the normal direction (encoded in red), but its velocity is slowed to 9 cm/s. Absence of flow in the portal vein (PV). Additional sign: large-caliber hepatic artery (A), arterial waveform
3) Intraluminal Changes
1)Acute portal or mesenteric vein thrombosis:
- Patient presents with clinical picture of Acute abdomen.
Echogenic filling defect
Vascular dilatation
Absence of color Doppler flow signals

Acute portal vein thrombosis. Mass in the portal vein (VP) is iso echoic to liver tissue (arrows). CDS shows no evidence of flow
2) Chronic Portal Vein Thrombosis

Chronic portal vein thrombosis (PVT) in the setting of a paraneoplastic syndrome. Hepatic metastases: very little increase in luminal diameter, intraluminal echoes in thrombosed portal vein segments. Intrahepatic portal vein is clear

Thanks for this great blog post it was really helpful to lots of are customers who were worried about there liver ultrasound and the results. This is a great blog keep up the work.
ReplyDeleteThat is not the falciform ligament on the first 2 drawing; it is the ligamental teres
ReplyDeleteIt proved to be Very helpful to me and I am sure to all the commentators here! Sonogram technologist
ReplyDelete